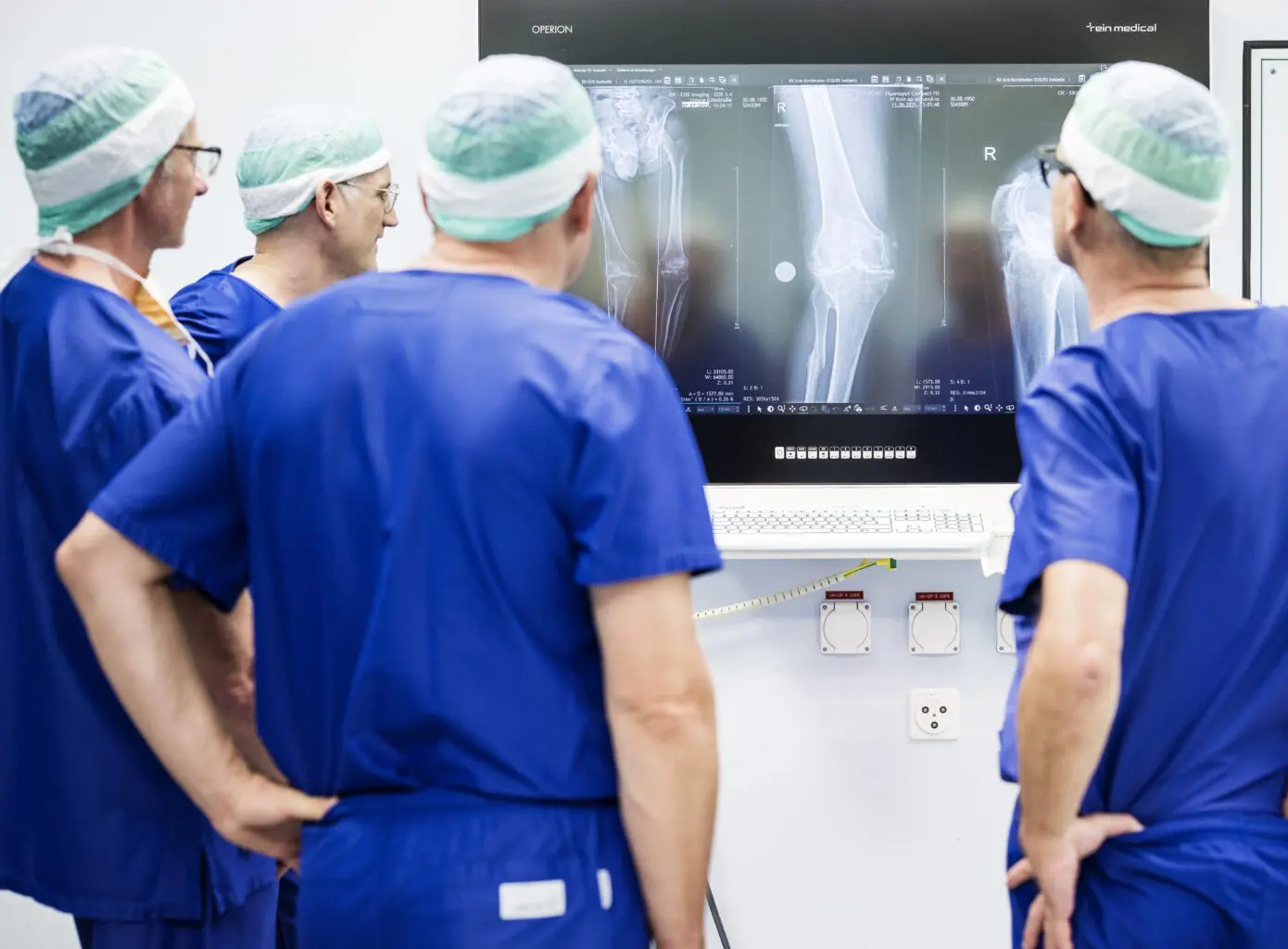
The MAKO surgical robot supports the surgeon in the exact implementation of this computer plan.
Individual 3D planning
In preparation for a MAKO operation, a computer tomography scan of the affected joint or leg is first carried out. This usually takes place around 2 weeks before the operation and is carried out at the Salem Hospital, as we have the certified equipment for this. The examination itself only takes a few minutes. Before the operation, a team of specialists will use these images to create a virtual, three-dimensional model of your joint on the computer and carry out initial planning of the operation. This model and the planning are then shown to the surgeon. The surgeon can follow all the planning steps and, if necessary, adapt or optimize the surgical planning to your needs.
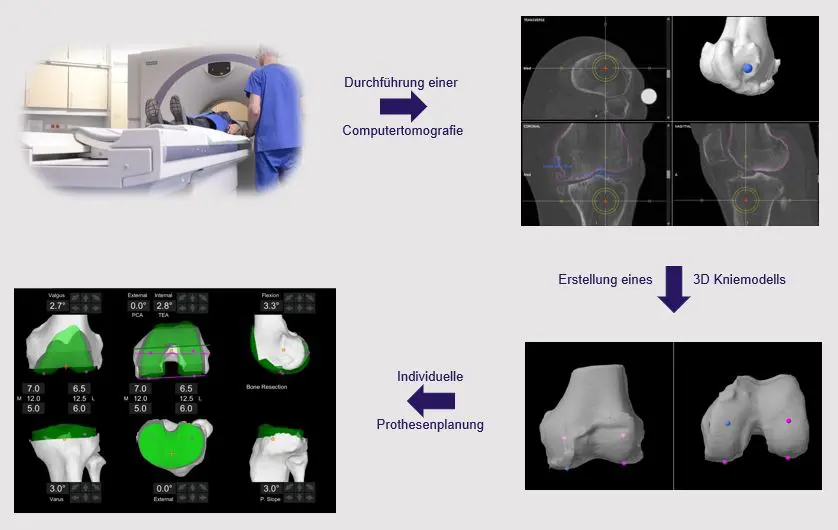
With this planning, the operation can begin. The entire operation preparation process is no different from our other standard procedures, especially with regard to anesthesia procedures or operation time. While you are still preparing for the operation, the computer in the operating theater will be started up and the robotic arm calibrated. This is done by a specially trained member of the manufacturer's staff, who accompanies each MAKO operation from start to finish. They are driven into the operating theater, where everything is already set up and prepared. Disinfection and draping are carried out with the utmost care, as with any other operation. The surgical approach and the presentation of the joint are not significantly different from other operations.
In the next step - and this is specific to all computer-assisted surgical procedures - optical markers are attached to the upper and lower leg bones or the pelvic bone. The navigation system with infrared camera uses these markers to recognize the position of your leg in space throughout the operation. The anatomy of your knee or hip joint is then compared with the 3D bone model in the computer using movements and tactile instruments. This entire process takes less than 5 minutes. You now have a very precise image of your bone anatomy in the computer.
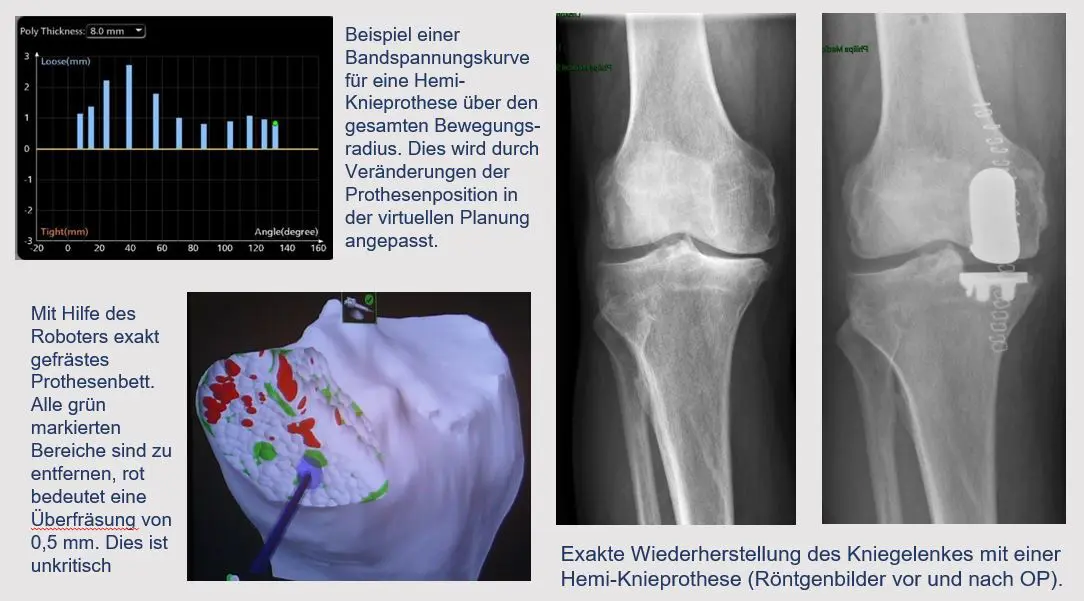
Fine-tuning the planning in the operation
However, information on the ligaments and soft tissue is still missing for the correct adjustment of the prosthetic components on the knee joint. In the next step, the ligament tension in different positions of the joint is also read into the system. To do this, the surgeon moves the joint passively and saves the ligament stability. The initial surgical plan is now checked in relation to the soft tissue. The aim is to reconstruct a joint that is stable over the entire range of motion with a movement sequence that is as natural as possible. The planning can be adapted accordingly and each individual parameter can be changed three-dimensionally in the 0.5 mm or 0.5° range.
At the hip joint, the aim is to reconstruct the exact leg length and the lever arms of the muscles. To do this, the leg length and the offset of the hip are measured before the prosthesis operation and then with a trial prosthesis. The optimum leg length and tension ratios can then be checked during the operation, also in relation to the opposite side, and gradually adjusted. With the help of a computer simulation, the range of motion can even be viewed and optimized by adjusting the position of the prosthesis.
Robot-assisted surgery
Only when this virtual planning has been optimized is the actual robot arm moved to the operating table and set up. The calibration is checked once again with an error tolerance of less than 0.5 mm. The MAKO robotic arm is now used to create the saw cuts or mill the prosthesis bed. The actual instrument is guided by the surgeon at all times. The robot only specifies the correct and planned sawing plane and prevents incorrect adjustment of the saw or burr. It also sets narrow limits for the instruments. Whenever the surgeon wants to leave the defined sawing area, the device stops automatically. This protects the surrounding soft tissue structures better than any hook. Once all the saw cuts have been made, the trial prosthesis can be inserted to check the correct fit and ligament stability once again.
This is objectively evaluated once again by the computer. If there are any deviations, a correction can be made with the system at any time. If everything goes according to plan, the original prosthesis is then inserted. This is followed by the usual wound closure and removal of the navigation aids. The follow-up treatment and rehabilitation corresponds to our standard follow-up treatment scheme, although we often observe faster rehabilitation due to the soft tissue-sparing technique.