On the day of the operation, the main focus is on good pain management and minimizing blood loss. Numerous measures are combined to achieve this.
Hospital admission
As a rule, you will be admitted to hospital on the day of the operation. You will be informed of the exact time directly by the hospital the day before. This is usually around 2.5 hours before the planned time of the operation. On admission, you should report directly to reception, where you will be given further assistance. Some preparations will then be made at the admission clinic.
The operation
You will then be taken directly to the operating room or to anesthesia preparation. There you will be met by your anesthesia colleagues.
The operation itself takes about 1 hour. In the case of partial anesthesia (spinal anesthesia), you can sleep or listen to music during the operation. You will not notice anything.
We use the minimally invasive, antero-lateral approach on the side of your thigh to access the hip joint. With the antero-lateral approach, muscles are no longer cut, but we use natural muscle gaps and pass between the muscles to the hip joint.
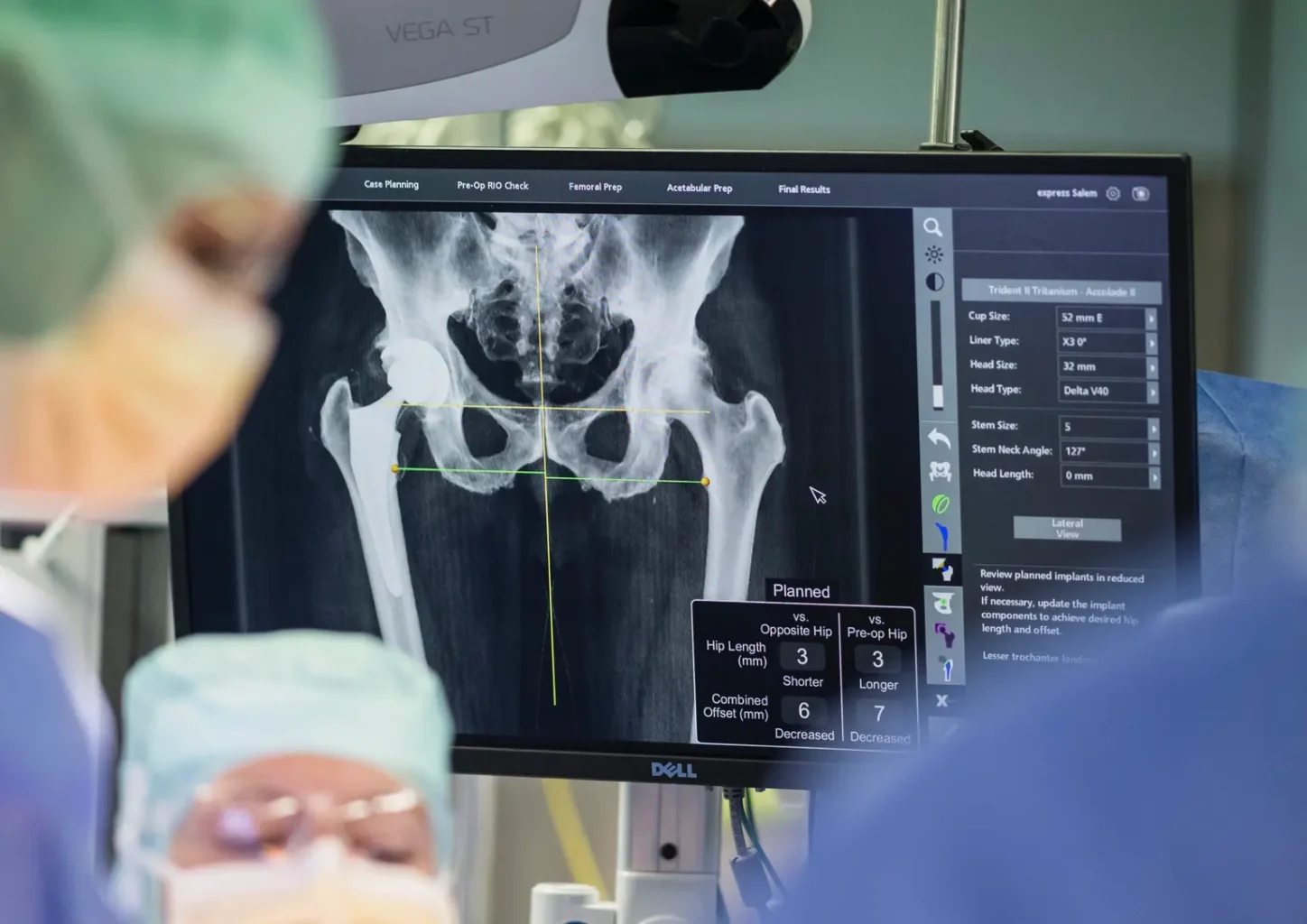
The preparation of the implant bed for the cup can be carried out with the help of the robot based on the previous computer planning. The original implant with the insert is also inserted with robotic assistance. The femur is then prepared for the stem component. The leg length is measured and adjusted with the robotic support we use.
An X-ray check is then carried out in the operating room so that you can be safely mobilized again with full weight-bearing in the afternoon.
At the end of the operation, the wound is sealed with a waterproof adhesive. The patient then goes to the recovery room for about 2 hours and then back to the department.
Optimal patient care around the operation
A key aspect of patient care is reducing blood loss and the risk of infection in order to minimize complications and promote recovery. Various measures are combined to achieve this.
- Antibacterial skin preparation with a shower gel
- Medication to minimize bleeding (tranexamic acid = Cyclokapron®).
- Lowering blood pressure during the operation
- Dispensing with drainage
- Antibacterial sealing of the wound with an adhesive
- Antibiotic shielding around the operation
Thanks to the combination of these measures, the average blood loss during hip replacement surgery is around 500 ml so that blood transfusions are generally no longer necessary today.
Prevention of dislocation of the hip
Thanks to the minimally invasive technique and robotic support, the risk of dislocation is very low (less than 0.5% with articon). You can sit normally right from the start (even on the toilet), bend the hip joint over 90° and sleep on your side. For patients at risk, we use special implants (bipolar heads) with additional dislocation protection.
Optimized pain therapy
The pain after hip prostheses is often well tolerated and rarely requires the use of stronger painkillers such as morphine derivatives. After surgery, standardized pain therapy is carried out according to a step-by-step scheme. You will receive basic therapy, usually Brufen® 3 times a day in combination with gastric protection. You will be asked several times a day about your pain level and the medication will be adjusted accordingly.
Mobilization and physiotherapy
Mobilization begins immediately after the operation, as soon as you have full feeling in your legs again and your circulation is stable.
The prosthesis is usually fully weight-bearing straight away and you will learn to walk with walking sticks in hospital. You receive physiotherapy once a day and are given exercises for self-therapy, which are also compiled in a brochure. You are encouraged to extend your range of movement every day.
In the first few days, the focus is entirely on gaining independence and mobility. Before discharge, you will also practise climbing stairs.
Avoidance of complications
A hip prosthesis implantation is a very standardized procedure with a very low risk of complications overall. The main aim is to prevent thromboses, falls and infections.
To prevent thrombosis, it is important to mobilize your joint and yourself as early as possible. You can do exercises to prevent thrombosis yourself by moving your toes and feet up and down in bed. You will also receive a daily injection to thin the blood (Fragmin). On discharge, the prophylaxis will be changed to a tablet (Xarelto® or Aspirin cardio ®), which you should take for 30 days after the operation.
In addition to the standard surgical measures, we use a special wound dressing similar to a second skin to prevent infection. This seals your wound and must NOT be changed. It is simply left in place for 2 weeks. From the 2nd day after the operation you can also shower with it. Stitch removal is no longer necessary with this special dressing.
Leaving the hospital
The hospital stay is usually 2-3 days. The following criteria must be met for discharge from hospital to home:
- Irritation-free, dry wound conditions
- Controlled pain
- Independent mobility with walking sticks
Hospital discharge is always by 9 a.m. (weekends by 10 a.m.).
In the week following discharge, you should continue with outpatient physiotherapy. Ideally, you should arrange your first appointments before you leave hospital. A wound check is scheduled 14 days after the operation. This can be done by your family doctor or by us in our consultation hours.